The need and demand for point-of-care ultrasound (POCUS) is increasing, and not just in the emergency department. However, the lack of affordable and efficient training solutions is a barrier to widespread adoption. Until Sonosim.
Scientific breakthroughs across medicine have become so frequent, time simply doesn't allow them all to be integrated into medical education. For example, despite the introduction of medical ultrasound in 1942, widespread adoption of point-of-care ultrasound (POCUS) has yet to occur. Providing sufficient ultrasound training to achieve ultrasound competency is a major barrier.¹ In fact, in 2020, the Joint Commission on Accreditation of Healthcare Organizations (JCAHO) cited “adoption of POCUS without necessary safeguards a major technology hazard.”²
POCUS is at a critical crossroads. Training resources and competency standards need to be bolstered for the benefits of clinical ultrasound to be realized. Expert consensus agreement has been reached on critical elements of ultrasound competency.³
What is Point-of-Care?
Point-of-care ultrasound (POCUS) refers to the use of portable ultrasonography at a patient’s bedside for diagnostic (symptom or sign-based examination) or therapeutic (image guidance) purposes.
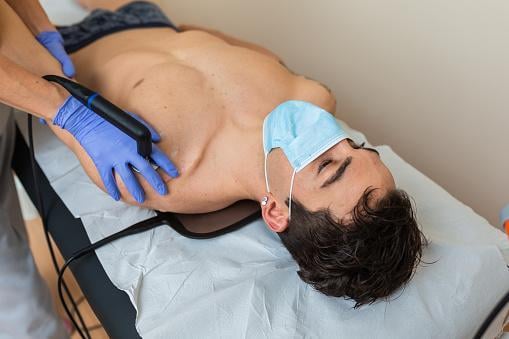
While traditional methods of performing a physical examination are of critical importance, healthcare practitioners that become skilled in the use of point-of-care ultrasonography become uniquely empowered.
As of 2020, an estimated 35% of the 222 medical schools in the United States have initiated ultrasound training programs.⁴ The challenge for these ultrasound educators is to deliver standardized ultrasound education and ultrasound competency. Simulation centers play a critical role. Simulation centers can leverage proven, validated, third-party educational platforms for standardized ultrasound education needed to achieve ultrasound competency.
Point-of-Care Improves Healthcare
Point-of-care ultrasonography improves healthcare. While traditional methods of performing a physical examination are of critical importance, healthcare practitioners that become skilled in the use of point-of-care ultrasonography become uniquely empowered to better care for patients. Point-of-care ultrasound has been proven to improve patient outcomes and experiences including, but not limited to:
- Providing faster diagnosis of time-sensitive critical conditions (e.g., leaking AAA, ruptured ectopic pregnancy)
- Minimizing delays in care (e.g., time to IV antibiotic administration due to lack of IV access)
- Diminishing procedural complications (e.g., iatrogenic pneumothorax following CVL placement or thoracentesis)
Point-of-care ultrasonography has the potential to save billions of dollars on an annual basis across health systems. It has the capacity to increase patient throughput via more accurate and timely clinical diagnoses, improve procedural efficacy, decrease complications, and limit pain and suffering. Advances in ultrasound technology, including improved ease of use, superior image quality, and lower-cost ultrasound units, have fueled the emergence of point-of-care ultrasonography.
👉 Related Read Ultrasound Training for Physicians: Why Your Practice Needs Ultrasound
Examples of faster diagnosis with point-of-care
The range of clinical applications that point-of-care ultrasound is being utilized for is rapidly expanding on a continuous basis. Looking for real-life examples of how point-of-care can improve diagnosis turnaround time? We thought you’d never ask.
- In patients with a swollen arm or leg, a deep vein thrombosis can easily be screened for at the bedside without having to anticoagulate the patient while waiting for an ultrasound.
- Differentiating simple cellulitis from the need to surgically drain an abscess has been shown to be superior with ultrasound.
- Long-bone fractures can be diagnosed and reduced under ultrasound guidance.
- Many times foreign bodies can be localized and removed without the need for fluoroscopic guidance.
- Needle-based procedures can be made safer and timelier when done under ultrasound guidance. This includes paracentesis, thoracentesis, arthrocentesis, pericardiocentesis, lumbar puncture, regional anesthesia, and vascular access.
- Conditions such as cardiac valvular disorders that are inferred by auscultation can be visualized and quantified by ultrasound. Time-sensitive definitive diagnoses, such as ruptured abdominal aortic aneurysms, are made in minutes rather than hours.
- Patients with flank pain or hematuria, where the kidneys can be evaluated for the presence of hydronephrosis, renal cysts, or distortion of the renal architecture consistent with a renal mass.
- The bladder can be assessed with ultrasound to estimate the volume and confirm ureteric expulsion of urine into the bladder using Doppler. The presence of these bladder jets confirms patency of the ureters, avoiding an unnecessary computed tomography (CT) scan.
Point-of-Care Barriers
The need and demand for ultrasonography training has grown in parallel to the expanded use of ultrasound technology. However, the primary barrier to future universal adoption of this operator-dependent “stethoscope of the future” is the lack of widespread, efficient, and affordable training solutions.
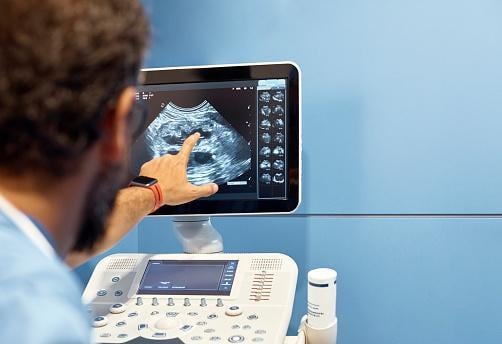
Point-of-Care Use Case
A study published in 2020 aimed to present the first, innovative, and structured POCUS program in neonatal–perinatal medicine field. In addition, they reviewed the availability of the POCUS training programs across different medical specialties.
In this study, Dr. Dalibor Kurepa recalls his recommended experience with SonoSim.
“In our institution, we selected online on-demand SonoSim (SonoSim; Santa Monica, CA) teaching modules. Our platform is customized with modules that cover didactic material pertaining to neonatal POC US applications. Didactic lectures include modules that cover US basics, anatomy and physiology, clinical pathology, and procedural US. A mastery test is administered at the end of each lecture. This peer-reviewed spectrum of lectures is supplemented by a virtual simulator that further enhances the material being presented. This software transforms a personal computer into a hands-on US training platform on a virtual patient. The USB-powered probe is an integral part of the system. Trainees have the opportunity to practice in a risk-free computer-generated environment. This method allows them to exercise their psychomotor skills, spatial understanding, and US image acquisition. While allowing “live” scanning, the system provides immediate expert tutoring and US probe positioning guidance. Additionally, access to didactic lectures and an ultrasound probe with the virtual simulator at the trainee’s convenience. Student performance is tracked online with simultaneous data feedback transferred to the training program educators’ dashboard. In addition to the platform modules, we formally present neonatal pathology-specific lectures that are not covered by the online platform (i.e., head US). These lectures are formal but interactive with an emphasis on developing required knowledge and confidence in US scanning.”
Ready to Implement Point-of-Care Ultrasound?
SonoSim can help with that. Providers are busy and time is a precious commodity. SonoSim Ultrasound Training Swas created to allow providers to access anytime, anywhere hands-on scanning practice with the SonoSim Probe on their personal computer. With SonoSim learners can avoid the cost, travel, and limited hands-on training experience associated with traditional ultrasound courses.
CTA button: I’m ready to learn ultrasound
References
¹ Soni NJ, Tierney DM, Jensen TP, et al. Certification of Point-of-Care Ultrasound Competency. J. Hosp. Med 2017;9;775-776. DOI:10.12788/jhm.2812
² Castro G. Top 10 health technology hazards for 2020. Oakbrook Terrace, IL: The Joint Commission, January 3, 2020 (https://www.jointcommission.org/resources/news-and-multimedia/blogs/dateline-tjc/2020/01/top-10-health-technology-hazards-for-2020/)
³ Tolsgaard MG, Todsen T, Sorensen JL, et al. International Multispecialty Consensus on How to Evaluate Ultrasound Competence: A Delphi Consensus Survey. Milanese S, ed. PLoS ONE. 2013;8(2):e57687. DOI:10.1371/journal.pone.0057687.
⁴ Diaz-Gomez JL, Mayo PH, Koenig SJ. Point-of-Care Ultrasonography. N Engl J Med 2021; 385:1593-1602. DOI: 10.1056/NEJMra1916062