Point-of-Care Ultrasound • POCUS
Challenges Abound for POCUS Learners
The challenges to learning and teaching ultrasound at the bedside are well-known and well-documented. Throughout medicine, practitioners know that point-of-care ultrasound can greatly speed up and increase the accuracy with which patients are diagnosed and treated.
However, learning and teaching POC ultrasound requires overcoming a lot of critical factors. You have to be able to overcome a lack of machines, a lack of ultrasound experts available at the right moment, a need for the right patients at the right time with the right pathology, the ability to create standardization of learning and repetition for learners... the list goes on.

Pros & Cons of Bedside Learning & Teaching
There is no better way to learn POCUS than having a qualified instructor take a learner with baseline ultrasound knowledge through a diligent ultrasound exam that helps inform medical decision-making. However, in reality, the lack of standardized access to pathology, qualified instructors, teaching moments, and access to ultrasound machines all combine to create massive obstacles to widespread POCUS competency. Combine with the lack of foundational ultrasound knowledge in learners, performance tracking, assessment, and feedback mechanisms and the barriers become a seemingly unsolvable puzzle.
Not Looking For POCUS Training?
Learning to Acquire & Read Ultrasound Images
Challenges Abound for POCUS Learners
Mastering point-of-care ultrasound (POCUS) can be an intimidating endeavor. This cutting-edge imaging method has gained popularity in clinical settings due to its numerous advantages over traditional methods. It is a non-invasive, portable solution that offers real-time imaging, allowing clinicians to interpret and quickly translate findings to patient care. However, there are several obstacles that care providers encounter when learning to perform ultrasound at the bedside in clinical practice.
One of the primary challenges lies in the variable & inconsistent exposure to patient pathology. Unlike radiologists who analyze countless scans daily, clinicians using POCUS may only come across a few cases each week. This scarcity can make it challenging to learn to acquire ultrasound images, identify abnormalities and develop a comprehensive understanding of what constitutes "normal" in ultrasound readings.
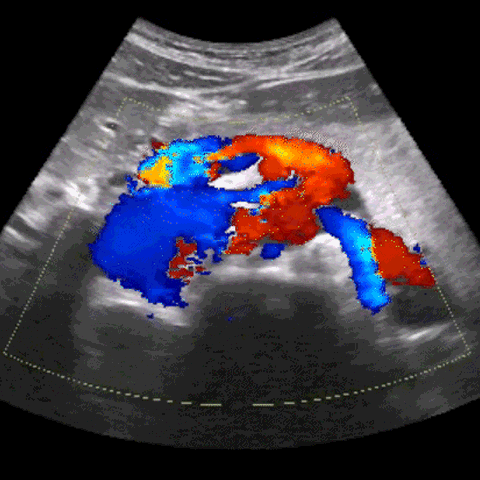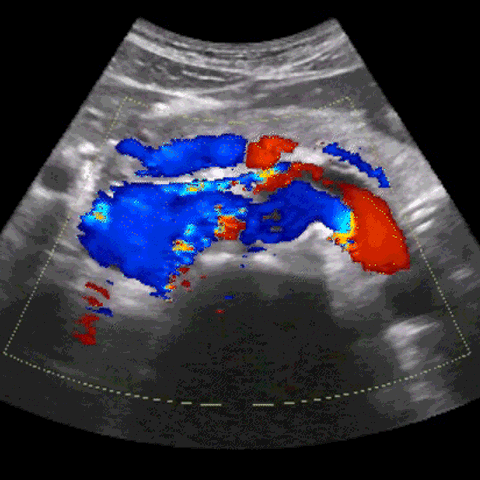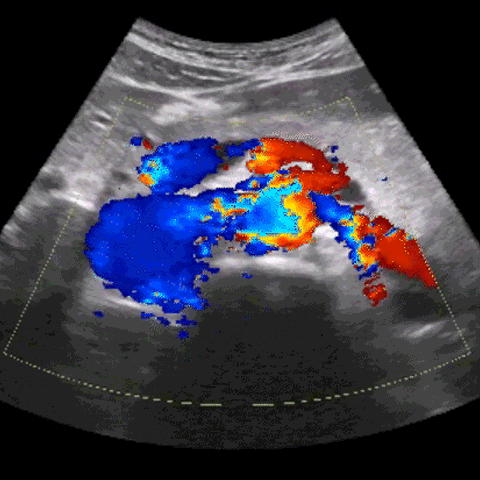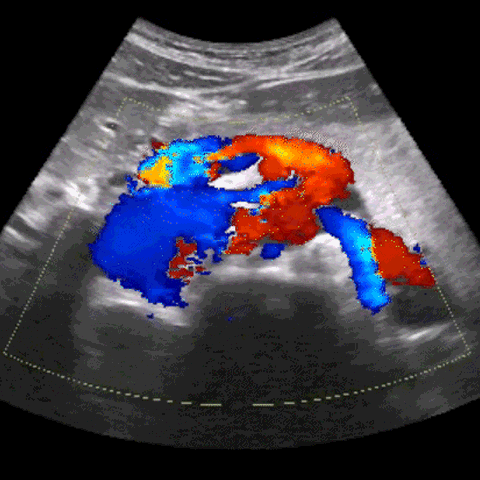
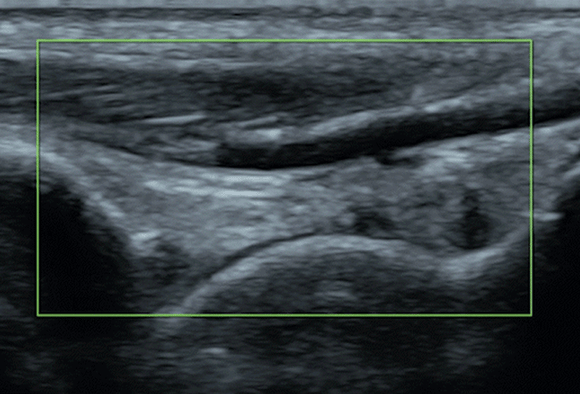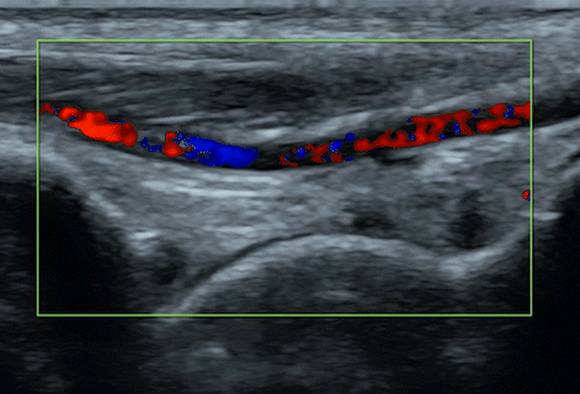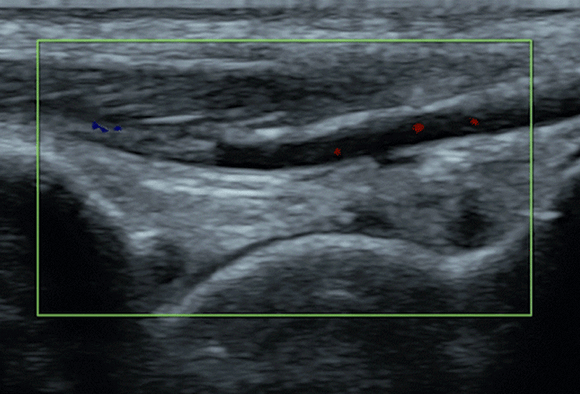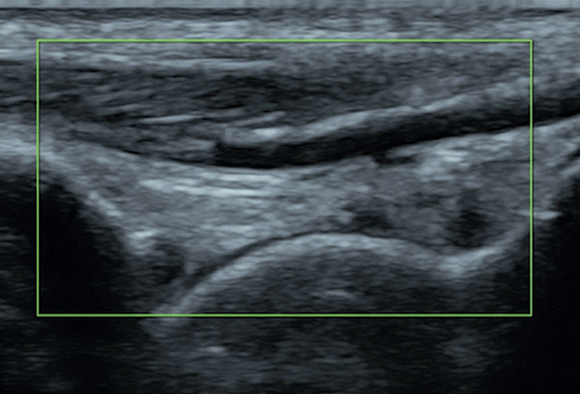
Consistently correct interpretation of ultrasound images also proves to be a formidable challenge. The intricate nature of anatomy and the lack of standardized protocols contribute to the difficulty in reliably interpreting ultrasound images. Distinguishing between normal and abnormal structures can be particularly challenging, especially when dealing with critically-ill patients. And, understanding how to use and/or overcome imaging artifacts, such as shadowing or reverberation, is a critical skill that adds to the complexity of ultrasound acquisition & interpretation.
Point-of-care ultrasound skill acquisition is also often compromised by the limited availability of ultrasound experts to provide feedback. The learning curve for ultrasound can be steep and protracted, and it may take some time before a novice is proficient enough to perform scans without supervision.
Finally, learning & teaching POCUS can be challenging because of time constraints that limit "teaching moments". Characterized by having an ultrasound machine, a patient with pathology, a learner, a qualified instructor, and the ability to engage in deliberate practice, teaching moments are rare. These teaching moments are critical and need to be repeated multiple times, and applied to each new ultrasound application a learner wishes to master.
.gif?width=600&height=400&name=dvr_20210122_0937_V3_gif%20(2).gif)

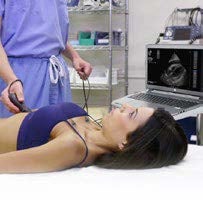
The machine may not be readily available to the learner at a critical teaching moment.

Getting enough ultrasound experts is often challenging and costly, plus availability at critical moments is near impossible.

Learners are confined to what patients present with during the hours they have a probe available.

Clinical bedside scanning often takes place in a chaotic environment. For the patient, pathology, expert, and machine to all line up to create a teaching moment is rare.

The needed repetition to learn is often not possible.

Adequate funding can be challenging to get.

How SonoSim Can Help
SonoSim complements bedside learning & accelerates the path to ultrasound competency.
SonoSim helps solve the puzzle of ultrasound competency by helping learners establish the baseline knowledge required to maximize the benefits of bedside clinical practice. With our ecosystem of ultrasound learning & teaching tools, we can serve a critical role for programs of all sorts in standardizing access to pathology and facilitating subsequent ultrasound education, training, and performance tracking.
SonoSim was built to help healthcare practitioners, program administrators, instructors, faculty, and others wanting to learn POCUS, overcome all these challenges. We do this through a proven methodology with an entire ecosystem of content, tools, and resources built up to make it the easiest way to learn & teach ultrasound. Using cloud- and laptop-based technology and advanced simulation capabilities, SonoSim provides self-paced content, tools, support, and resources to help overcome the barriers to ultrasound learning.
Click on the video below for a full overview of the SonoSim Ultrasound Learning & Teaching Ecosystem, or click on any one of the elements below for a more detailed overview of what is included.
Flexible Learning Pathways
A customizable ecosystem for everyone
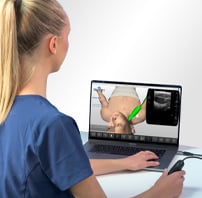
Innovative ultrasound simulation environment. Master scanning skills with the SonoSimulator. Accessible anytime, anywhere.
A growing library of Challenge Cases enable learners to continually scan new pathologies & acquire new skills.
Access scanning assignments to teach imaging protocols published by professional society guidelines, including AIUM, CAAHEP, ACEP, and more.
The SonoSim Wave
An Ultrasound Insights Newsletter
Get the latest trends in ultrasound training, education, & applications delivered to your inbox.