Self-Paced, Remote Ultrasound Learning
While we aren't a school ourselves, we support many academic programs & sonography schools with robust, realistic, yet remote ultrasound training capabilities.
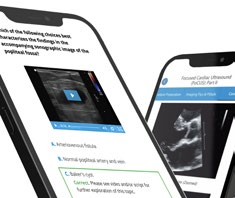
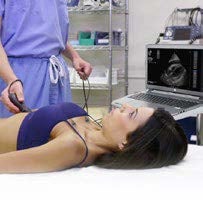
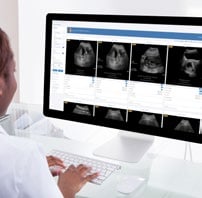
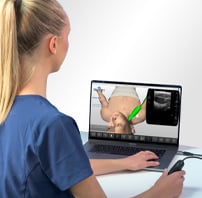
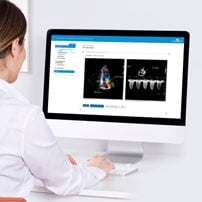
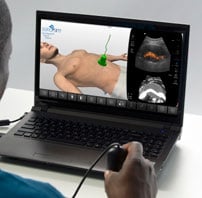
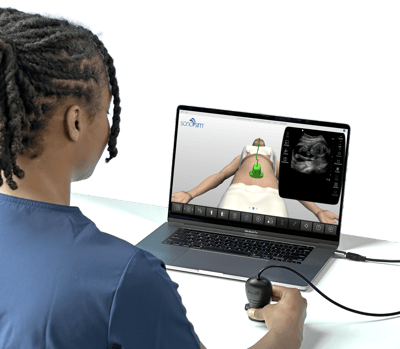
SonoSim is a self-paced remote ultrasound learning platform that combines online multimedia courses and hands-on scanning of real patient cases applied to virtual patients. Courses are interactive and cloud-based, including video, case studies & more. SonoSim members also get access to our patented SonoSimulator software & probe that allow access to unlimited scanning of real pathologic cases on a laptop.
Looking for a Sonography School?
We're glad you're considering a career in ultrasound. We aren't a school ourselves, but we work with a lot of them and are happy to support you in a variety of ways. We have resources for you to help you find a sonography school. We also have a discounted student membership that can be purchased while you are enrolled.
Calling All Medical & Sonography Students!
Ultrasound Enthusiasts! Interns & Residents! Prospective Sonographers!
We Have Great Options for You!
Tell Your Program About SonoSim
You're a techie in the coolest way!
Looking for an Ultrasound School?
Here are some resources for you.
Medical Students! Looking to Excel in Rotations?
We're thrilled to hear you're passionate about ultrasound. We are too! We work with a lot of medical schools to advance learning overall with ultrasound, but some students often want more comprehensive ultrasound training than some schools provide. That's why we're offering a discounted student membership that can be purchased while you are enrolled. If you sign up and dedicate time to learning ultrasound, it will advance your understanding of patient anatomy and pathologies, as well as your performance during clinical rotations.
Take advantage of educational discounts up to 12 months after graduation.**
SonoSim appreciates the challenges you face in developing ultrasound knowledge and skills.
Now, with our student/recent graduate membership, you can access all the courses, scanning cases, & study tools SonoSim offers for up to 12 months after graduation at special discounted pricing.**
We want to support you as you embark on your career. Prepare for boards or refresh your knowledge regularly. Study for certification exams like the SPI exam or use our Courses & QuestionBank to refresh your knowledge. Build a portfolio of solid ultrasound imagery in the SonoSimulator® for job applications, credentialing and more. And study on-the-go with our mobile app, SPI Test Prep, and QuestionBank functionality.
The Student All Access SonoSim Membership is not eligible for CME/CEU credit.
Get full access to the entire SonoSim Ecosystem, which is growing all the time:
- Online Ultrasound Training Courses (80+)
- Ultrasound Videos (6500+)
- Ultrasound Case Studies (1000+)
- Knowledge Check Questions (1500+)
- Mastery Test Questions (1600+)
- SonoSimulator Software & Probe for Virtual Hands-on Scanning (1)
- Virtually Scan Real Cases (1000s of windows)
- Scanning Practice on Real Pathology (Unlimited)
- Image Acquisition & Interpretation Guidance (Unlimited)
- SPI Test Prep Quizzes & Mock Exams (800+ Questions)
- Certificate of Completion (80+)
- Personal Ultrasound Image Portfolio (Unlimited)
- & More

Check the search feature of CAAHEP  ︎
︎
CAAHEP accredits many types of allied health programs including DMS programs. You can search for CAAHEP-accredited programs on their website. Be sure to select "Professions" --> DMS and Echocardiography (in Cardiology Technology) when conducting your search.
Check the State-by-State Listings on Ultrasound Schools Info  ︎
︎
ARDMS conducts sonography certification exams. Check out their student tips page.
Traditional ultrasound training methods can present hurdles to achieving ultrasound competency. This often can limit in-depth ultrasound learning in school as well as in medical practice. These barriers can be effectively mitigated through ultrasound simulation with SonoSim.

Limited Ultrasound- Trained Faculty

Inconsistent Access to Pathology

Lack of Ultrasound Machines

No Performance Assessment Resources

Restricted Time in Curriculum

Funding
SonoSim's Comprehensive Ultrasound Training Ecosystem
Self-Paced Remote Ultrasound Learning & Scanning that Supports Students

The SonoSim Wave
An Ultrasound Insights Newsletter
Get the latest trends in ultrasound training, education, & applications delivered to your inbox.
**Eligibility Criteria
To be eligible for the SonoSim Student - Graduate All Access Membership, you must be either:
1) a current student1 at an accredited diagnostic medical sonography (DMS) program, medical school, or
2) a recent graduate2, less than 12 months from graduation, from a DMS, medical residency program, or undergraduate medical school that offered SonoSim to you while you were enrolled.
1 Proof of active enrollment and projected or actual graduation date required.
2 Renewable annually while you are in school and for 1 year following graduation.