Can We Agree on Cardiac Tamponade? Exploring POCUS Interpretation Among Emergency Physicians
Explore how POCUS training affects cardiac tamponade diagnosis reliability among emergency physicians, revealing both potential and challenges in...
Take advantage of blended learning. Deliver online didatic lectures, while reserving valuable classroom time for engaging and interactive teaching moments.

Medical educators must consider many factors when seeking to integrate ultrasound training into their medical programs. Upon defining the scope of an ultrasound curriculum, ultrasound program leaders need the capacity to deliver standardized ultrasound education to large numbers of medical students. Students need hands-on training to master ultrasound image acquisition, interpretation, and application of findings toward patient care. These educational objectives are balanced against the preferences of how today’s medical students want to learn.
Learners today demand engaging, interactive educational experiences in place of traditional textbook-based instruction. Medical students prefer to independently access learning resources on-demand, such as short-form content that is accessible across a variety of platforms including laptops, tablets, and smartphones (Bahner et al., Hempel et al., Huynh et al., Tarique et al., Leszczyński et al.).
Blended learning is a learning paradigm that “combines face-to-face instruction with computer-mediated instruction” (Bonk and Graham). The methodology can be used to deliver self-directed, ultrasound training that combines cloud-based didactic instruction, hands-on training with simulation, and performance assessment. A blended learning approach has the collateral benefit of helping medical schools satisfy the Liaison Committee on Medical Education (LCME) self-directed learning mandates while supporting remote instruction and distance learning (Sakai et al.).
Obstacles to delivering quality ultrasound education within medical schools stem from both ultrasound instruction itself and curriculum integration. These barriers include a paucity of qualified ultrasound technicians, access to patients with pathologic conditions, practice environments, financial resources to support training and assessment, and an already densely-packed undergraduate medical education curricula (Bahner et al., Dinh et al., Ma et al.).
|
Barriers to Ultrasound Instruction |
Barriers to Ultrasound Curriculum Integration |
|
Ultrasound technology |
Lack of funding for machines & maintenance |
|
Qualified instructor |
Limited faculty time for instruction |
|
Patient with pathology |
Restricted clinical access to patients |
|
A teaching moment |
An overfilled medical school curriculum |
|
Refresher training |
Lack of resources for assessment |
Figure 1.
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) pandemic lockdowns and continued fears of disease transmission create additional barriers to ultrasound learning by cutting off an entire generation of ultrasound learners from accessing clinical training sites. Ultrasound learners, including medical students and residents, have lost readily available access to bedside ultrasound training across a variety of clinical settings. Ultrasound educators will need to identify novel methods to overcome this added barrier to ultrasound instruction.
A traditional approach to teaching medical procedures involves a “see one, do one, teach one” approach (Vozenilek et al.). As ultrasound training requirements increase, the availability of ultrasound-trained instructors quickly becomes a rate-limiting factor (Siegel-Richman & Kendall). This is particularly relevant as institutions seek to integrate longitudinal ultrasound curricula across multiple years (i.e. MS1-MS4) of undergraduate medical education.
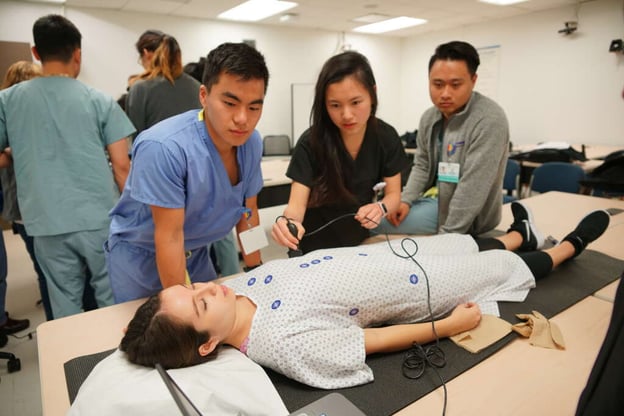 Peer-to-peer instruction using SonoSim LiveScan® to facilitate integrating ultrasound findings into medical decision-making (scenario-based training)
Peer-to-peer instruction using SonoSim LiveScan® to facilitate integrating ultrasound findings into medical decision-making (scenario-based training)
Many medical schools have applied a peer-to-peer (student-to-student) approach to ultrasound training to overcome the shortage of qualified instructors and reduce curricular expenses (Tarique et al.). Preliminary studies have demonstrated that peer instructors can successfully train fellow students on select introductory ultrasound applications (Ahn et al., Celebi et al., Jeppesen & Bahner, Tarique et al.).
Validation of these respective approaches will require additional rigorous studies that analyze ultrasound competency in medical students trained through these teaching methods. It is vital to precisely define the scope of ultrasound competency across students and establish validated instructional and performance assessment methodology, given the potential harm arising from inaccurate ultrasound diagnoses and incorrectly performed ultrasound-guided procedures (Moore & Copel).
Blended learning, or the “flipped classroom” approach to ultrasound education and training, is the idea that learning will take place in a traditional classroom, lab, or face-to-face setting, but is also coupled with independent study and online learning on the student’s own time. Blended learning has grown rapidly and is now widely used in education. Specifically, online learning has quickly become a popular resource for health education due to its ability to transcend space and time boundaries, while also providing reusable and up-to-date information often delivered in an engaging and interactive multimedia format.

Online learning has quickly become a popular resource for health education due to its ability to transcend space and time boundaries.
Studies have demonstrated that online learning is as effective as live classroom instruction and bypasses the physical limitations of students and instructors needing to be together at a central location, at a given time (Gray & Tobin, Lie et al.). According to Gray and Tobin, it’s important to consider that both students and faculty have a hand in a healthy blended learning approach to clinical education. Faculty must be open to the incorporation of novel elements into the curriculum and students must understand that face-to-face time with experienced educators truly shapes both their clinical skills and how they will present as health professionals in the future. Together, they can set forth the cultural shift necessary to provide a positive, forward-thinking approach to bedside ultrasound education and training.
Studies have identified the key tactical components needed to successfully implement blended learning (Bonk & Graham, Gray & Tobin, Liu et al., Osguthorpe & Graham., Saritepeci M & Cakir). Applying these principles toward a blended learning approach for ultrasound instruction involves the following considerations:
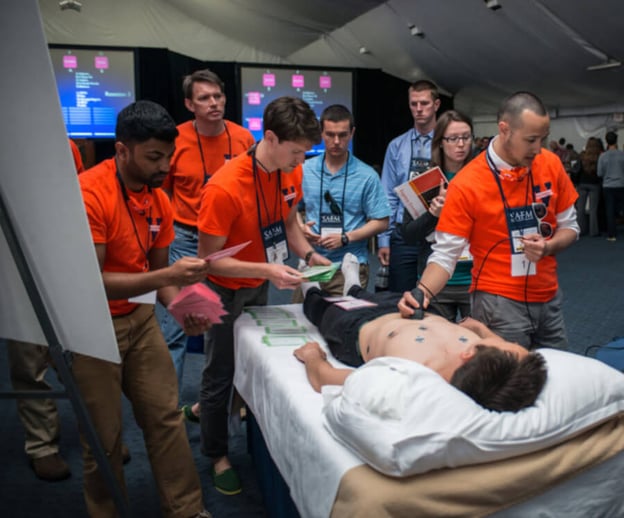 Medical students participating in SonoGames® using SonoSim LiveScan® to apply ultrasound findings toward medical decision-making in a fun, competitive environment
Medical students participating in SonoGames® using SonoSim LiveScan® to apply ultrasound findings toward medical decision-making in a fun, competitive environment
Blended learning serves as a proven-effective approach for ultrasound education amongst medical students. In a study at Eastern Virginia Medical School (EVMS), first-year medical students participated in a simulation-enhanced ultrasonography curriculum as part of the comprehensive curricular integration of ultrasound skills. The goal was to assess student knowledge and performance of ultrasound and determine student satisfaction with the integrated curriculum.
Students attended one-hour lectures from an experienced instructor, followed by small breakout simulated scanning sessions where they received face-to-face demonstrations by faculty. They then participated in 45-minute scanning sessions with standardized patients in which they saved ultrasound images and received feedback. In the following weeks, students would resume scanning in 45-minute sessions following their anatomy labs to reinforce their skills and engage in peer-to-peer interaction.
The study showed that scores nearly doubled in the post-test versus the pre-test, and nearly 83% of students could adequately capture an image. Additionally, students reported that the ultrasound curriculum was an asset to their medical education, and they would enjoy engaging with ultrasound training in the future. The balance of carefully curated in-person instruction coupled with strategic, independent follow-up scanning sessions proved to be a successful and beneficial blended learning approach at EVMS.
Training solutions must have the capacity to teach learners ultrasound image acquisition and interpretation across a variety of pathologic conditions. The use of real ultrasound imagery during instruction is critical to teaching learners about ultrasound artifacts that are important determinants of accurate image interpretation. Students will need methods to adequately capture their ultrasound knowledge, while clinical ultrasound instructors will need the ability to track student progress, manage assignments, assess student performance, and provide feedback.
As medical schools consider how to build an efficient and effective pathway for students to learn ultrasound, the growth of validated ultrasound training is available to support their efforts (Chung et al., Gottlieb et al., Maw et al., Monti & Perreault, Paddock et al.). Key components to support blended learning include the capabilities to deliver didactic instruction in an on-demand and mobile-optimized format to match the preferences of today’s learners.
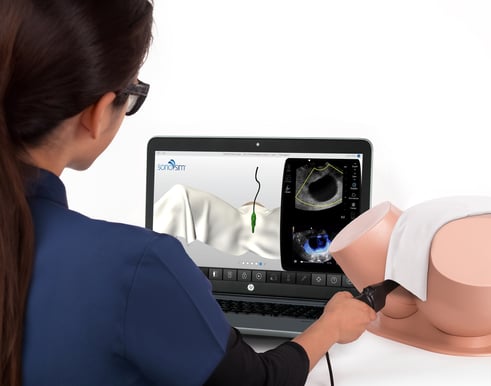 A validated blended learning approach to ultrasound training includes on-demand didactic instruction and remote practice scanning, which enhances live training with ultrasound educators
A validated blended learning approach to ultrasound training includes on-demand didactic instruction and remote practice scanning, which enhances live training with ultrasound educators
Recent advances in medical simulation provide performance tracking supported by artificial intelligence. These help ultrasound educators manage their ultrasound training programs. Features include automated didactic knowledge assessment, individual student declarative knowledge tracking, real-time ultrasound image acquisition guidance, automated assessment of ultrasound task performance, real-time feedback supported by a virtual instructor, and performance feedback by program administrators.
These collective advances provide institutions with the support required to effectively build a comprehensive ultrasound curriculum that delivers high-quality standardized ultrasound instruction to large numbers of medical students. They also reduce the time burden of administering an ultrasound program. This provides talented ultrasound leaders with the time needed to discover novel clinical applications of bedside ultrasound, as well as develop their ultrasound training programs.
The ability of medical schools to successfully integrate ultrasound education into current curricula is vital to the growth and development of today’s medical students. By leveraging a win-win blended learning approach to learning ultrasound, institutions can provide their students with the autonomy to build a foundation on their own time through engaging online training solutions. Faculty will then be able to enhance learning by teaching students through high-impact live-instruction sessions, thus providing a deeper, more efficient, and rewarding learning experience. As a result, students will be better prepared for the competitive medical education journey ahead.
Explore how POCUS training affects cardiac tamponade diagnosis reliability among emergency physicians, revealing both potential and challenges in...
Learn how SonoSim responds to AIUM's new OBGYN ultrasound training recommendations by providing residency programs with competency-based learning...
Advances in ultrasound machines are only as effective as an operator's ability to use them. Learn how SonoSim is using simulation to break those...
Get the latest trends in ultrasound training, education, & applications delivered to your inbox.
Have Questions?
Click here to chat!